Cervical myelopathy results from the interruption of the normal neural circuitry of the spinal cord. Trauma, infectious or inflammatory processes, tumors, or degenerative processes including spondylosis and intervertebral disc herniation can cause myelopathy. It is the last group of causes that are of particular significance to the neurosurgeon or spinal surgeon. Cervical myelopathy secondary to degeneration is called “cervical spondylotic myelopathy”. This is a result from degenerative spondylosis and the risk increases with age.
The spinal cord is encased in an enclosed bony tube. Surrounding the spinal cord is a layer of fluid, which provides protection from trauma and allows flexibility of the neck. In some instatnces, people are born with a smaller-than-average spinal canal; this is called “congenital cervical spinal stenosis”. Stenosis is a general term for narrowing.
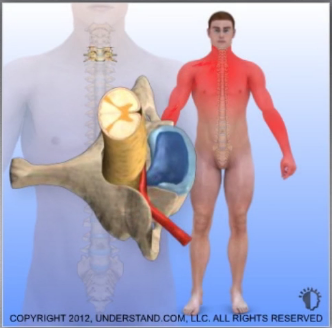
The cervical spinal canal may become narrowed over time due to degenerative changes within the spine. Bone spurs (osteophytes), disc bulges, and thickened ligaments may develop and encroach on the spinal canal. In some cases, the space normally surrounding the spinal cord may be severely compromised causing pressure on the spinal cord.
The symptoms of cervical myelopathy depend on the level of the spinal cord involved and the degree of involvement. Symptoms may include: numbness of the hands, clumsiness of the hands, arm weakness, hand weakness, leg stiffness (“walking like a robot”), loss of balance, frequent falls, loss of fine motor skills and urinary urgency. Neck pain may also be present but is frequently not a significant complaint.
The key to the treatment of cervical spondylotic myelopathy is to remove the pressure from the spinal cord. The goal of surgery is to prevent the progression of symptoms; clinical improvement may or may not occur.
Surgical procedures to decompress the spinal cord include approaches from the front of the neck (anterior cervical discectomy and fusion, anterior cervical corpectomy), from the back of the neck (cervical laminectomy, cervical laminectomy and fusion) and combined procedures in which both an anterior and a posterior approach are used. The exact procedure performed is based on the location and degree of the stenosis and the overall alignment of the cervical spine, but many factors are considered in the decision.

Dr. Ram R. Vasudevan, MD, FAANS
Austin NeuroSpine PLLC
5300 Bee Cave Road, Building 1,
Suite 220 Austin, TX 78746
Phone: (512) 640-0010
Monday: 8:00 AM – 5:00 PM
Tuesday: 8:00 AM – 5:00 PM
Wednesday: 8:00 AM – 5:00 PM
Thursday: 8:00 AM – 5:00 PM
Friday: 8:00 AM – 5:00 PM
Saturday: Closed
Sunday: Closed
© 2023 Austin NeuroSpine PLLC. All rights reserved.